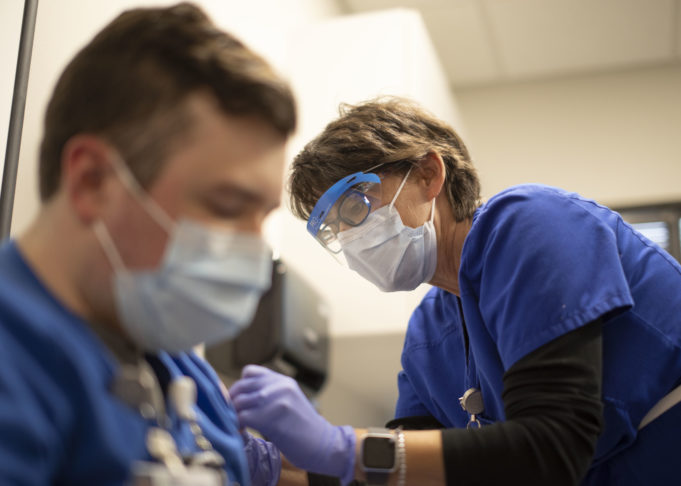
Wednesday’s COVID-19 vaccine felt like “hope in a bottle,” said Dr. Kerim Razack, partner with Texas Pulmonary & Critical Care Consultants at Texas Health Southwest. As one of three critical care doctors at his southwest Fort Worth hospital, Dr. Razack has worked six weeks straight. Since March, he estimates that his critical care team has seen upwards of 100 local residents die from COVID-19, often after struggling for up to several weeks on ventilators.
Hospitalized patients are now treated with steroids, convalescent plasma (taken from patients who have recovered from COVID-19) and the antiviral treatment remdesivir, he said. Patients who continue to decline are placed on ventilators as a last resort.
“If we are putting someone on a ventilator, they are extremely sick,” Dr. Razack said. “If you are bad enough to need the ventilator, your chances of dying are 90 to 95%. That’s why the mood in the ICU is so grim. Everybody knows that as soon as this patient ends up on the ventilator, in two, three, or six weeks, they will likely die from this. If they survive, it could take months to learn how to walk and eat again.”

After eight months of treating patients for a disease that has claimed the lives of 306,427 Americans, Dr. Razack sees the COVID-19 vaccine rollout as the “beginning of the end” to the worst pandemic the world has seen in a century. The physician said he felt no symptoms for several hours after receiving the Pfizer vaccine.
“At about eight hours, my arm was a little sore, and I felt a little achy, kinda like when you are starting to get the flu,” he said. The next morning, “I woke up feeling fine.”
On Tuesday, 5,850 doses of the COVID-19 vaccine arrived at Texas Health’s central pharmacy. Small boxes containing the inoculations were stored at -94 degrees Fahrenheit as required by the manufacturer. Before shots are administered, the vaccine must be thawed and then diluted, said a spokesperson for Texas Health Resources, which has 28 hospitals.
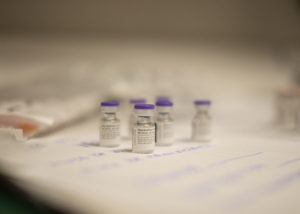
Barclay Berdan, Texas Health CEO, said his “team members are exhausted from nine months of providing intensive care to seriously ill patients with COVID-19, but despite that weariness, they continue to care for patients and their families each day. The vaccine will help protect these heroes as they continue to serve the people in our communities.”
On December 11, the Food and Drug Administration (FDA) issued the first emergency use authorization for a COVID-19 vaccine, this one from Pfizer. FDA Commissioner Stephen Hahn said the authorization “follows an open and transparent review process that included input from independent scientific and public health experts and a thorough evaluation by the agency’s career scientists to ensure this vaccine met FDA’s rigorous, scientific standards for safety, effectiveness, and manufacturing quality needed to support emergency use authorization.”
The Texas Department of State Health Services (DSHS) said that four sites received 19,500 doses of the Pfizer vaccine Monday morning, and 19 sites received 75,075 doses on Tuesday as part of what the state is calling Week 1 of distribution. By Monday, DSHS plans to deliver 224,250 doses to 110 providers across the state.

The arrival of the first batches of Pfizer vaccines comes at a time when North Texas and the state are experiencing a surge in COVID-19 infections and deaths. Texas now has 1,367,965 confirmed COVID-19 cases, according to DSHS. Tarrant County has 107,721 confirmed cases and 1,205 COVID-19-related deaths.
Thursday, 30 frontline workers received COVID-19 vaccines at Cook Children’s, a hospital spokesperson said. The initial recipients included “doctors and nurses who work with COVID-19 patients as well as employees who may be in close contact with patients and families such as environmental service workers, members of Cook Children’s Teddy Bear Transport Team, security, lab, and food and nutrition employees.”
The day was “emotional,” said Debbie Boudreaux, assistant vice president of nursing at Cook Children’s, “because we’ve waited so long for this pandemic to end. This has been a team effort from the very beginning, with our COVID-19 Command Center working tirelessly to adapt to all the changes we’ve had to make to keep our employees, patients, and families safe.”
Medical City Fort Worth spokesperson Tommy Dold said his 320-bed facility has not received vaccines from the state as of Wednesday. Tarrant County Public Health spokesperson Brian Murnahan said TCPH has not received COVID-19 vaccines because the treatments are going to frontline healthcare workers first. DSHS allocation principles outline state priorities for vaccine administration. Health care workers, particularly those working on the frontline, are prioritized. Residents of long-term care facilities and hospice workers are also included in the state’s first phase of vaccine rollouts.
The Moderna vaccine is set to become the second vaccine to see mass distribution in the United States. An FDA advisory committee recently endorsed the vaccine, meaning full FDA approval could come as soon as today with distribution beginning Monday. Unlike the Pfizer vaccine, Moderna’s preventative treatments can be stored in normal freezers, which will allow for easier distribution to rural areas in Texas.
In light of the ongoing vaccination efforts, Dr. Anthony Fauci, the nation’s go-to official on infectious diseases, said the United States could see the early stages of herd immunity by as early as late spring. Gov. Greg Abbott said Texans can expect widespread distribution of the COVID-19 vaccine by March.