In May 2012, Fort Worth Police Officer Jody Timmons was chasing an assault suspect over a chain-link fence and fell on her right side. When she fell, she fractured her collarbone and tore the meniscus in her knee, and a disc in her neck slipped out so far it pushed against her spinal cord.
“When I was standing there, my knee started hurting, and I felt a pain in my shoulder that radiated down to my fingers,” she said.
She hasn’t been able to work since that day. CorVel initially denied her request for surgery on the basis that she had not yet tried enough physical therapy. Eventually, the company approved a surgery that fixed her knee, but CorVel denied that her neck issues were caused by her fall.
![FEATURE_2 Timmons: “You reach a point where you feel like giving up, which is what [CorVel] wants.”](https://www.fwweekly.com/wp-content/uploads/2013/12/FEATURE_22-200x300.jpg)
Since then, the company has repeatedly denied permission for the various treatments recommended by her doctors for both her neck and shoulder. But because her injury occurred more than a year ago, the city of Fort Worth expects her to get back to work any day now.
It was her CorVel claims manager, Terry Marshall, who denied the claim on Timmons’ neck injuries, not a doctor. In fact, even CorVel’s doctor agreed that she needed surgery on her shoulder and neck, but that finding was overruled by Marshall.
CorVel did not respond to questions about the medical qualifications of its caseworkers. However, on the company’s website, medical training is not listed as a requirement for the position.
“With everything being denied, denied, denied, you basically feel helpless,” said Timmons. “You reach a point where you feel like giving up, which is what [CorVel] wants you to do.”
Though Timmons has officially been back on active duty since Sept. 1, she has yet to return to work. She has been able to stay home only by burning through her sick days and other paid days off. She takes pain pills daily to manage what she described as a constant pain throughout her body. The medication and stress have caused her to fall into depression, so she now takes an antidepressant in addition to the pain medication. The amalgam of pills has affected her short-term memory, which she described as being “shot.”
The ordeal has also strained her marriage, she said.
In receiving treatment, she has been shadowed by what’s known as a nurse facilitator, who acts as a medical liaison for CorVel, following patients as they see their doctors.
“I had [a nurse] who asked to go to my doctors’ visits, and I refused,” she said. “I didn’t want her there while I was getting treatment. So she’d have to make her own appointments.”
In October, Timmons filed a complaint against CorVel with the Texas Insurance Commission, but she hasn’t heard back from them. She filed for an injury leave extension with the city so she could have more time to recover but characterized that process as another maze of red tape and bureaucratic gymnastics.
The city employees “were horrible with me,” she said. The police department said she couldn’t get another extension unless she was recovering from another surgery — which she was trying to get for her neck but which had been denied by CorVel.
Timmons and her husband have hired an attorney and plan to pursue legal action.
Her story is typical of the reports the Weekly heard from various city staffers who have dealt with CorVel.
One tactic those staffers said CorVel commonly uses to deny medical treatment is to claim that an injury was caused by a degenerative condition, not the incident that precipitated the workers’ compensation claim.
In Gillette’s case, his back pain became degenerative because of the constant strain he’s put on his body while working for the police department, he said.
“The only reason I have a degener-ative condition is because of what I’ve been doing in my line of employment,” he said.
Over the course of his career, Gillette has been treated for a ruptured disc and had vertebrae fused together, and he suffers on-again, off-again back pain.
After his most recent injury, his doctor recommended a neural stimulator — like a pacemaker for the spine — and physical therapy.
After waiting almost five months, Gillette called CorVel and found out that his request had been denied because his doctor allegedly didn’t do a peer-to-peer interview with CorVel’s doctor. His doctor assured Gillette that he had contacted CorVel and that no one had responded to his calls.
Eventually, CorVel responded by asking for a second opinion. In such cases, the patient can go see the specialist of his or her choice. The doctor he saw for the second opinion recommended another procedure that would essentially burn the nerves between his discs so he won’t feel the pain of them rubbing together.
His doctor requested permission for that procedure several weeks ago and still hasn’t heard back.
“I’ve never been through this rigmarole with my other injuries,” said Gillette. “I’ve had broken bones, legs injured, ankles rebuilt, etc. I’m pretty well bionic by now.
“I had a doctor tell me that [CorVel’s] intent is to do the bare minimum,” he said. In the doctor’s experience, Gillette said, “Their goal is to get you the minimum amount of treatment at the minimal amount of cost, regardless of your condition.”
Gillette said he still feels a dull, persistent pain in his back and is not well enough to return to duty.
“On a 10-scale, I constantly run about a two or three,” he said. “I’ll go from the couch to the chair to the bed, then stand up for a while, then walk around. I drive my wife nuts.”
Another officer, who asked not to be named, said another third-party administrator also tried to deny his claim based on his “degenerative” condition.
In 1997 the officer was rear-ended by a drunk driver while stopped at a traffic light. He ruptured two discs in his neck and needed to have three vertebrae fused together. Contract Claim Services, the firm handling the city’s workers’ compensation claims at the time, approved, and the surgery was performed.
A decade later, the repaired discs broke apart, causing him severe pain. This time, Contract Claim Services refused to OK the surgery, saying the problem was degenerative and thus not covered.
The officer paid more than $2,000 for various tests to prove that his condition was not degenerative. He sued to force the city to pay for the surgery. On the morning, 18 months later, when the case was to go to trial, Contract Claim Services dropped their opposition and agreed that the problem was work-related and therefore covered.
The officer was seen by a doctor selected by Contract Claim Services who recommended new surgery. But this time, the claims company responded that surgery wouldn’t fix the problem and denied the claim again.
CorVel inherited the problem but still hasn’t approved the surgery. The officer said CorVel officials have told him the company considers the matter settled. Now, he said, CorVel won’t return his calls.
The officer said he has been in serious pain since 2007. It’s often so bad, he said, that he can’t get out of bed.
If injured workers use their personal insurance to see a doctor for medical procedures related to their injury, they run the risk that their cases will no longer be considered workplace injury.
“I’m just stuck,” the officer said. “I can’t go to the doctor on my regular insurance because [the injury] is work-related, and I can’t go to a workers’ comp doctor because they just won’t let me. It needs to be fixed.”
Gillette expressed the frustration the other officers say they feel.
“This could have been done months ago,” he said. “I could have been back to work last July or August, but now I’m looking at February or March.”
********






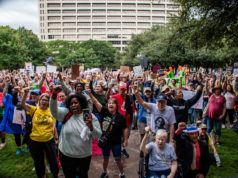




FWW might wish to explore the percentage of “recommended” spinal surgeries which are successful. (definition: substantial permanent recovery from pain and ability to return to full time work status). I would suggest that upon investigation, the author (and the patients described above ) might concur that the ‘best” spinal surgery is NO spinal surgery. Patients should follow conservative treatment recommendations for physical therapy, weight loss, etc prior to undergoing an irreversible and potentially risky surgery. My problem with spine surgeons and orthopedic surgeons in general is that they financially control every aspect of WC treatment evaluation to an alarmingly self serving degree. Many own shares in clinics, hospitals surgery centers and MRis outright –so it is no surprise that a diagnosis supporting a multi thousand dollar surgery (some up to $75,000-100,000) is reached. What happens if the patient is a victim of failed back surgery syndrome? (.ie. the surgery does not work). Frequently those patients are thrown on the disability ash pile with a few addictions to strong pain medications as an added burden( at public expense). I do feel that the Health Insurance industry is corrupt and complicit in some of this as well (in a self serving way), but this topic is complex and deserves mor in depth analysis.
When you have three different types of imaging studies and conservative measures have failed, you have the surgery. PT will not fix a blown disk or torn ligament. It sounds like JN is the one with the big red DENIED stamp. If someone has never had to navigate the hell Chip is enduring, they have no right to speak on the subject. It’s a nightmare realized.
Can you email me? I’d love to pick your brain on some things. Thanks, eric [at] fwweekly.com
I have emailed you.
CorVel wouldn’t return any phone calls? Did you call them at midnight? 6 pm on a Saturday?
We called them at every possible hour of every day during the week for two weeks.
They knew we called and why.
This subject was well covered by Brettt Shipp on WFAA in 2003, and resulted in re -formating (reorganizing) the TWCC by removing an obvious 75 year old insurance industry advocate (former insurance agency owner-I believe) as head of TWCC with a former Texas Medical Board administrator (also elderly) who allegedly over saw medical board abuses of the health insurance industry( which was instrumental in filing anonymous complaints against innocent physicians who sought more comprehensive care for their HMO and worker’s comp patients). If anything, the abuses are even worse now, in the opinion of some. The insurance industry remains unchallenged by either party and has a huge lobbying presence locally and nationally. They will argue that their profits are “minimal” but they continue to have escalating annual retrurns, and multi-million dollar CEOs. One economist pointed out that if the WC and other insurance companies were not profitable-they would have such exponential growth in numbers of companies, TPAs and other associated support organizations. It would probably be best if there was limited self referral by certain members of the medical community,but re-imbursement limitations are responsible for that ethical dilemma as well. In short, Edward CorVel doesn’t even need to acknowledge that you exist, because they are in complete control.
Chronic pain/ can’t find the pain go to Dr. Howard Cohen PRIDE- Dallas. Treats a lot of injured soldiers (IED’s). The ONLY Dr. That has helped me.
Eff the city, department, and Corvel. JN/DD I’ve fought the nightmare for 5 1/2 years. DD, surgeons will LIE…2 year statute of limitations medical malpractice…period. JN, Sunshine Act (8/13) is supposed to expose these hidden financial ties between Dr. and corporations.
FWPD, AFLAC does NOT cover on duty injuries for p/t jobs. Also, sign up for long term disability insurance with the city. Crap happens, stay safe;)
I bet the Mayor didn’t have this problem when she fell off her bike and bumped her head…SMH
Hmmmmmmmmm.
I guess one conclusion that FWPD officers could make from all this is to not get hurt on duty, whatever that takes. You wonder how much better Sgt Gillette might be if he hadn’t risked his health trying to subdue a miscreant citizen of a city who views its employees as disposable rather than valuable.
Anyway, Sgt Gillette can now “endure” his job related, pain infused, well-deserved, involuntary retirement……oh wait, the Mayor and Council messed that up for the City’s “most valuable resources” too.
The worker s comp system has more shady characters and sub plots than a Charles Dickens novel. The insurance industry is quite powerful and has an extensive lobby. In the G H W Bush presidency , doctors were forced into a unique sort of “antitrust’ category which would not allow collective or essentially individual bargaining with health insurance companies. All independent physician reimbursements could be prorated on Medicare rates (which are not very high). This allows for escalating profits by “not for profit” hospitals (which successfully argued that they take a “hit” with indigent care–but charge everybody else three to ten times the going rate), pharmaceutical companies-(cost of research don’t you know), and Health insurers(who never fail to make incredible profits annually) Any so called “reform” is aimed at further marginalizing physicians income–ignoring the other primary three cost driving industries. (Is it any coincidence that these “profitable” industries all support ACA- Obamacare?) Workers comp in Texas was extracted from the PI attorneys provenance in the 1990s by the legislature under the “any willing provider” guise. In other words, if you were an injured worker, you did not need to sue your boss, you could go to any physician for an honest evaluation. Which was fair enough umtil these rights were erroded during the Perry years when worker’s comp insurers decided to get TPAs (third party administrators) to terrorize doctors and workers by extracting money from the physicians re-imbursements ( for unspecified “administrative” work–like doing nothing but attaching their names to the physicians reimbursement check and extracting10-15% for NO function e.g.) and denials of medical procedures and payments. As if the physicians were not demoralized enough, the TWCC (essentially a bureaucratic arm of the insurance comapanies) and the TDI (which is useless) teamed with the medical board to look for “overutilizing physicians”–in other words-physicians who had more workers comp patients than the insurance industry thought they should have. Filing anonymous complaints with the medical board to get rid of the pesky docs. The surgical docs decided to diversify and bought shares in hospitals, surgery and imaging centers to offset surgical procedure income loss(who can blame them?) The insurance companies see the end game of essentially employing these docs in the next decade or so and assuming control of their practices until they can make a profitable exit (merger acquisition etc). Independent docs are worn out by the insurance company tactics and really do not want to be on the phone all day for phoney “peer to peer ” consults with paid ins co employees -for little reward and refer their patients to the surgical docs (who have found a way to make a profit). This leaves the patient in limbo. CorVel has marketed their “package” to cities and large businesses under the guise of “exclusivity” which means they only allow a certain number of “providers” in their network–this essentially further slows the evaluation process for the patients (sound familiar-like ACA-ACO, etc.?). The cities and businesses pay less in premiums. Are the providers the “best”? Some would say,not…
Limiting the pool of providers and keeping inactive or deceased providers on a roster of providers while denying enrollment to potentially new and interested providers (saying the provider pool is full)– is a time honored con game of all health insurers. This limits the injured or ill parties access to care and makes the insurance companies more profitable. This is also the chosen “tact” of insurance companies under ACA-Obamacare under the ACO paradigm. Also who “judges” the “quality” of the provider pool? (Your good buddies in the insurance industry and government) How reassuring…
After reading this article I was first amazed that the worker’s comp program was CONTRACTED out in the first place. That this is happening in Texas does not surprise me, sad to say. The whole point of worker’s compensation programs is to get the worker back to work, if possible, as soon as possible, The fact that this contractor is not doing that by stalling surgeries & playing phone games is a waste of the taxpayer’s money as well as causing personal hardships to the affected employees. I work for the federal government & I thought our OWCP had some issues but this is unreal. The city employees need to take this to a higher level and beyond if needed as well as litigation.
Yep, they denied my claim for knee surgery after mangling my knee kicking a door in on a call… They were terrible to deal with. Glad I finally got it fixed, on my own dime.
Welcome to the BIG state and local Government-Health Insurance Complex! BTW Mary the Dept of Labor workers comp insurance is one of the most difficult in the nation to deal with!
I can see that the liberal leaning FWW is working pretty fast to “bury” this “cover” issue (another more maleable subject has already appeared) ;It is clearly not going the FWW socialistic (one payer system) way! I hope that the injured parties featured above are not feeling “used”. Too bad that the authors and editors could not build on previous investigative journalists’ work to actually reveal the truth. (That WOULD be asking a great deal, I suppose). My advice to patients is: Do not depend on your insurance company or your employer to take care of you. Seek several second opinions, ask around. Don’t depend upon some charismatic provider to send you into an irreversible medical situation which you may regret!
The paper had an early deadline so we wouldn’t have to work Christmas Eve and Christmas day.
Hello,
I am a line of duty disabled deputy sheriff out of Minnesota. As I read this article, I could not help but to get furious. I have been disabled since 1986 after the squad that I was operating was struck head on by a drunk driver.
Texas is not the only state that this kind of crap goes on. Minnesota can stand along side Texas in the way that the county that I was working for when I was injured. I had never had to deal with the workman comp system until then and I had a rude awakening.
When I was injured, I thought that I would be taken care of medically. I could not have been any more wrong.
I could write a book here of what all I went through and the results that I now have to deal with each and every waking second of every day. When I get to thinking about it, I have to be careful as I have a bad heart condition of which I can lay the cause to the lack of medical care that I received for my injuries.
My heart condition started when I was trying to get approval from the work comp overseer to get a mri done for what the doctor thought was a increase in pain contributed to a worsening of my condition from the injuries sustained in the accident. I called and called and called leaving messages with the company and after over a week of calling begging for permission to get the tests done, could not take the increased pain any longer and went into the ER at about five am one morning and explained to them about the need for a mri, they put me in a room and started to check me and all of a sudden, the nurses and doctor went ballistic. It ended up that I had been having a heart attack the entire time. I ended up having a quad by pass and over the years since, have had to deal with atrophy of my hands, arms, neck and upper back from the injuries that the county actually had the nerve to say were not there and had accused me of faking my injuries. My heart was damaged by the heart attack or I should say heart attacks as the doctors could not say how many I had suffered through while begging the company to get the mri done!
During that time, my heart continued to deteriorate and in the fall of 2010, while at a funreal the guy that was the sheriff while I was trying t get help, came up to me and jumped on my back and started to hit me, I was shocked. I went down to my knees because I felt my heart start to flutter. Finally he let me alone. It was embarrassing as there were sworen officers who just stood by and watched even though I was looking into their eyes and trying to get them to stop him. They did nothing. Then about four months later, with my heart going in and out of the flutter feeling and causing me to have to go down to my knees to avoid falling, I suffered another heart attack which caused me to die three times in one night. Fortunately, I was at the hospital when that happened and they were able to get me back.
I attribute the last heart attack also to the then retired sheriff who jumped on me. I still can not believe that he did that.
After he had done that, there was a dinner for the deceased and the guy came up and started to tell me that the atrophy of my upper extremities was all the result of getting older?!? The latest doctor who finally gave a crap about the atrophy which by now was very obvious, would have argued that point with the guy for sure. I was trying to swallow some food but the fluttering made it hard to swallow and I started to choke and he turned and walked away. Thank the lord that I had a glass of water to wash the food down.
It really is a sad state of affairs when it comes to how injured officers are cared for in this country. I would suspect that my story is not the only horror story in Minnesota.
I knew that the retired sheriff did not like me as I had supported a fellow who had run against him for the office of the sheriff. I knew that he had been unhappy about that but it had been at least six years since and I thought that he would have grown past that by then. As a matter of fact, when he walked up to me, I expected that he was going to shake my hand and not jump on top of me and start beating on me! After all this was in a church and at a funeral!!! I feel my heart starting to pound hard so I have to stop. Like I stated earlier, this is just a small part of how I was treated after having a legitament injury while on duty.
Also, in my case, I have to believe that the county would have preferred that I had died in the accident as it too would have been much less expensive for them. Even though, I had to pay for most of my care or I would have died a long time ago.
When I hear a politician say that injured officers are taken care of, I have to go away from where ever I am to avoid getting to worked up. As you can probably tell, my mind was also effected over the years as well. I try to think straight but sometimes when I get upset over all that happened since 1986, I get lost.
The worst about all of this is that my loved ones have had to watch my deterioration over the years and it is obvious that all of what has been done to me is going to cut my life short. It was very hard to come back in 2010 and I am afraid that I do not have enough strength to go through that kind of thing again.
Thank you
This article exemplifies how worker’s compensation cases are handled in Texas. Employers have the luxury of hiding behind their insurance carriers. They can cut worker’s compensation costs by choosing the lowest cost provider and at the same time separate themselves from the injured worker. Medical care is sacrificed for cost savings. Injured workers are given endless denials instead of treatment.
Texas legislature has acknowledged that worker’s compensation system is broken but fails to enact any real legislation to actually help injured workers. The recent Texas Supreme Court decision (Texas Mutual Ins. Co. v. Ruttiger) further demonstrates how inured worker’s rights continue to be eroded. This decision prevents bad faith or unfair practice claims against worker’s compensation insurance carriers. Tortious conduct by an insurance carrier will now go on unchecked and clears a path for them to act with impunity.
I am a police officer employed for an agency near Austin. I sustained a training/work related injury in 2011 which resulted in a herniated cervical disc. I have been subjected to a deluge of bureaucratic red tape. The Texas workers compensation system is so convoluted with procedures which are designed to outright deny cases involving any type of spine surgery. My case is similar to three other officers at my agency.
My case is currently scheduled for a benefit review conference (BRC) and a contested case hearing (CCH), requiring costly attorney fees. I have no other recourse but to hire an independent attorney since the Texas Department of Insurance (TDI) – Office of Injured Employee Counsel’s (OIEC) Ombudsman Program does not provide licensed attorneys to help injured workers. I previously contacted an ombudsman and was not impressed. OIEC is staffed with “qualified” personnel who have completed a “training program” who can “guide” you through the process. No thanks, I rather be represented by someone who is versed in statutory and case law. I really believe that the insurance carrier attorneys, the Division of Worker’s Compensation (DWC), or even TDI will not respect you if you are not duly represented by an attorney.
My employer’s insurance carrier requested a designated doctor’s (DD) exam whereby an “independent doctor “, or general practitioner, rendered an opinion not based in a field of specialty/experience but according to official disability guidelines (ODG). The DD completely disregarded my complaints of pain and my treating doctors’ recommendation for surgery. The DD stated that I was at MMI and no further treatment could be offered. I have appealed this decision and now waiting for a BRC.
While waiting for my BRC, my treating doctor has sent requests for surgery which have been met by peer review denials (X3). “Independent doctors” who do not examine me, but again review ODG, which explicitly does not recommend surgery for a majority of spinal injuries. Using ODG simplifies the process of the peer review and makes it easier to deny surgery. My doctor tries to appeal. which is referred to TASB, who forwards to an independent review organization (IRO), who then ultimately forwards my case to another designated doctor who quotes (verbatim) the denial of the previous peer review doctors. I have appealed this decision and now waiting for a CCH.
I have failed all other conservative and pain management (epidural injection) options. So in the mean time, I just have to deal with the neck pain and the sleepless nights caused by my arms going numb. Hopefully some day I will get approved for surgery before the pain medications cause serious kidney/liver problems or even worse, permanent/irreversible nerve damage from a herniated disc.
The insurance carrier is hoping that I will eventually give up this exhaustive process, like my other fellow officers who eventually used their private insurance and paid the $3000 out of pocket deductible.
I feel a personal injustice has been done and I am not going to give up this fight.
Official Disability Guidelines:
http://www.worklossdatainstitute.verioiponly.com/odgtwclist.htm
This article illustrates the folly of those who believe that their employer, workers comp or other health insurers will take care of you. In recent decades health providers have been reduced by government and insurance industry lobbyists to mere servants of the system (by insurance industry design). I would say that if you have the out of pocket deductible and a private insurance plan, this would be the time to use it…
It’s a scam . Was diagnosed with back strain when I told occumed my hip hurt . Did injections in my back but it never stopped my hip from hurting …. 6 months later they sent me to another doc and found I had avascular necrosis and needed a hip replacement. Hahaha the ins co instantly tried to close the case did the BRC then the dd and all the hoops to jump through . Hired a lawyer and prevailed at my extent of injury cch on nov 18 2014. I was injured July 1 2013. It is now 2015 and still can’t get in to see a surgeon. The carrier was ordered to pay . Big deal we are just cattle to feed the ins company. You can be proud of Texas all you want just don’t get hurt. The people who think it’s not a scam are not hurt . If you think you are important just get hurt on the job . You will be made to feel like a criminal. My advice is if you get hurt on the job get away from it go to the doctor and use your own insurance. Workers comp is a joke.
It’s a scam . Was diagnosed with back strain when I told occumed my hip hurt . Did injections in my back but it never stopped my hip from hurting …. 6 months later they sent me to another doc and found I had avascular necrosis and needed a hip replacement. Hahaha the ins co instantly tried to close the case did the BRC then the dd and all the hoops to jump through . Hired a lawyer and prevailed at my extent of injury cch on nov 18 2014. I was injured July 1 2013. It is now 2015 and still can’t get in to see a surgeon. The carrier was ordered to pay . Big deal we are just cattle to feed the ins company. You can be proud of Texas all you want just don’t get hurt. The people who think it’s not a scam are not hurt . If you think you are important just get hurt on the job . You will be made to feel like a criminal. My advice is if you get hurt on the job get away from it go to the doctor and use your own insurance.
It’s a scam . Was diagnosed with back strain when I told occumed my hip hurt . Did injections in my back but it never stopped my hip from hurting …. 6 months later they sent me to another doc and found I had avascular necrosis and needed a hip replacement. Hahaha the ins co instantly tried to close the case did the BRC then the dd and all the hoops to jump through . Hired a lawyer and prevailed at my extent of injury cch on nov 18 2014. I was injured July 1 2013. It is now 2015 and still can’t get in to see a surgeon. The carrier was ordered to pay . Big deal we are just cattle to feed the ins company. You can be proud of Texas all you want just don’t get hurt. The people who think it’s not a scam are not hurt . If you think you are important just get hurt on the job . You will be made to feel like a criminal
It’s a scam . Was diagnosed with back strain when I told occumed my hip hurt . Did injections in my back but it never stopped my hip from hurting …. 6 months later they sent me to another doc and found I had avascular necrosis and needed a hip replacement. Hahaha the ins co instantly tried to close the case did the BRC then the dd and all the hoops to jump through . Hired a lawyer and prevailed at my extent of injury cch on nov 18 2014. I was injured July 1 2013. It is now 2015 and still can’t get in to see a surgeon. The carrier was ordered to pay .
What a scam
Makes me furious. Do away with Corvel….allow the officers to utilize the insurance company the FWPD offers its employee as benefit. No hands in the pockets and will save alot of money and manpower. Take care of your people and they will take care if you. Pisses me off to see so many lazy people ride the welfare train abd we cant provide PROPER AND TIMELY medical care for those who protect and serve us. Might just start seeing more officer involved shootings because they cant effing run after them cause of an injury not treated/claim denied. Well im hoping a corvel employee needs the assistance of a FWPD officer and the officer DECLINES assistance in fear of an on the job injury. But we all know that will not happen because officers are driven by HONOR and INTEGRITY. ….something CORVEL will NEVER have.
I got a head injury at work 1/9/12… Witnessed slip and fall backwards on ice while working for WyndhamWorldwide in California. #TBI. Return to work denied repeatedly, no interactive process without doctor release,,,no doctor released without medically necessary care… Corvel costly denials for nearly 2 years.
First year treatment received was a few chiropractic sessions and a few clinical psychology sessions. Second year included six physical therapy treatments. Third-year included some speech therapy occupational therapy physical therapy and acupuncture. The first year the defense firm and adjuster of CNA denied medical care. Since February 2013 CorVel has obliged the carrier with false reports harassment of doctors and of course denials of medical care. I just got a new package of non-recommendations. For properly recommended medically necessary treatments.
An Injured law-enforcement officer, on one of the discussion boards of national Association of Injured and disabled workers, commented that Injured Workers Must start naming names and filing complaints.
Here’s my story… ask about Worker’s Comp. gravy trains http://askaboutworkerscompgravytrainsnow.com/list-of-posts/
It’s time for class action… Can Fort Worth ask the department of justice to pretty please help the people of America? Who is next?
Ok. That’s it. I’m drafting a complaint to declare the TX WC act unconstitutional before the federal court. Will ask for class action status. Who’s with me?
Daniel Montes
Texas Citizen Plaintiff
Plantoperationsdirector@gmail.com
There are a little bit of thread hanging
out but other than that, it is exactly the same. The new regime will abandon the concession system and shift to production sharing contracts.
As Petrobras is the leader in the development of the subsalt area in Brazil, a major part of the investment in the region is expected
to come from the company.
Adult Packages: The adult packages are one of the most popular and oft subscribed packages of the DISH Network.
You are going to need at least that long to see the difference that they
will make. They have only lost once in league so far 2015 and Wednesday visit to
West Ham United, who is ninth but has five games without a win.
Different company same story for The City of Fort Worth. I feel that if treatment was approved for my injuries a while ago, I would have been back on the streets, not getting worse with all the denials. The last time I spoke with my York case manager, she told me “its your own body, you can do what you want with your own body, out of your own pocket”.
Maybe There should be an updated story